Welcome to Jiangsu Yigao Medical
Welcome to Jiangsu Yigao Medical
 E-MAIL:[email protected]
E-MAIL:[email protected]

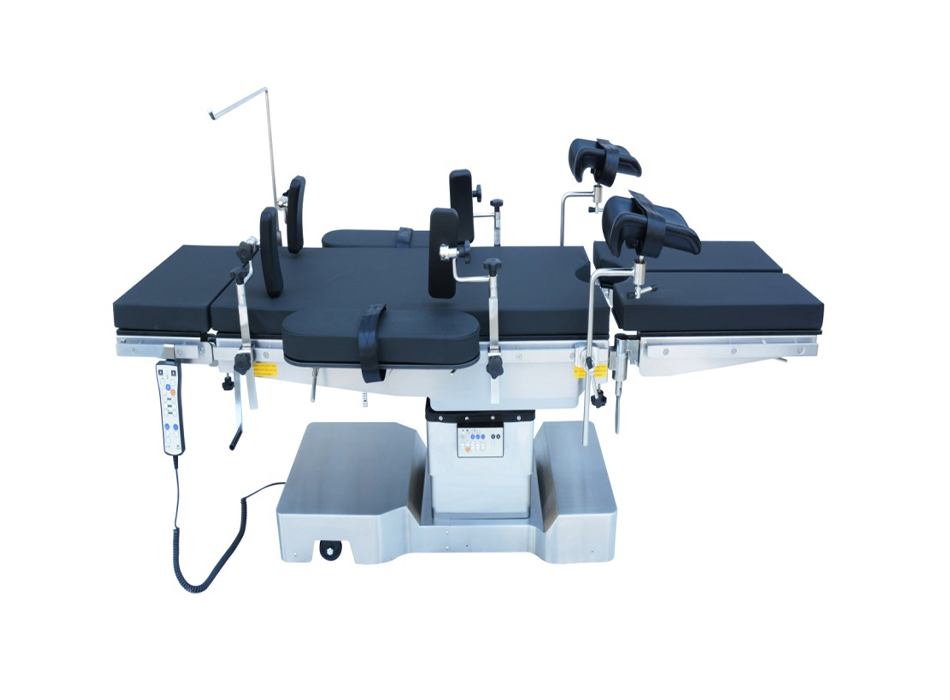
An operation table (also called a surgical table or operating table) is the central piece of equipment in any surgical suite — it supports the patient in precise, adjustable positions throughout a procedure and directly affects surgical access, patient safety, and team ergonomics. The three main types are electro-hydraulic operation tables, electric operation tables, and manual operation tables, each suited to different surgical volumes, budgets, and procedural requirements. For most modern hospitals performing mixed surgical caseloads, an electro-hydraulic or fully electric table is the correct choice. Manual tables remain valuable in lower-volume facilities, developing-region hospitals, and backup configurations. This guide explains every critical dimension of selecting, using, and maintaining an operation table.
Understanding the fundamental drive mechanism of each table type is the starting point for any procurement or clinical decision. The drive system determines positioning speed, precision, noise level, maintenance requirements, and suitability for different surgical disciplines.
Electro-hydraulic tables use an electric motor to drive a hydraulic pump, which in turn powers hydraulic cylinders to move each table section. This combination delivers smooth, high-force movement with excellent load stability. The hydraulic system provides natural damping — preventing sudden drops or jerky repositioning — which is critical when a patient is under general anesthesia. Most electro-hydraulic tables support patient loads of 250–450 kg, with heavy-duty bariatric variants rated to 500 kg or more. The Trendelenburg and reverse Trendelenburg range is typically ±30° to ±40°, and lateral tilt reaches ±20° to ±25°.
The primary limitation is dependence on both electrical power and hydraulic fluid integrity. A power failure during surgery requires a battery backup system (most modern units include 8–12 hours of battery operation) and hydraulic fluid must be inspected and changed on a scheduled maintenance cycle, typically every 2,000 operating hours or annually.
Fully electric tables replace hydraulic actuators with electric linear actuators on each table section. This eliminates hydraulic fluid entirely, removing the risk of fluid leaks in the sterile field and reducing scheduled maintenance demands. Electric tables offer highly precise positioning — movement increments as fine as 1 mm for height adjustment — and are generally quieter than electro-hydraulic systems. Load capacity is slightly lower than electro-hydraulic models, typically 200–350 kg, though premium models reach 450 kg.
Electric tables are particularly favored in orthopedic, neurosurgical, and minimally invasive surgery suites where precise, repeatable positioning is essential. Their compatibility with imaging equipment — particularly carbon fiber tabletops that are radiolucent across the full length — is a significant clinical advantage.
Manual operation tables use mechanical mechanisms — hand cranks, gas springs, or mechanical hydraulic pumps operated by hand — to adjust table position. They have no electrical components, making them immune to power failures, extremely durable in resource-limited settings, and straightforward to service. The trade-off is that repositioning requires physical effort from OR staff and takes longer than motorized adjustment. Typical load ratings are 150–250 kg, and the range of motion is generally more limited than motorized tables.
Manual tables are highly appropriate for general surgery, minor procedures, outpatient surgical centers with tight budgets, and facilities in regions where reliable electrical supply cannot be guaranteed. Their total cost of ownership is significantly lower than motorized tables, with purchase prices typically 60–80% lower than comparable electro-hydraulic units.
The following table provides a structured comparison of the three operation table types across the parameters most important for clinical and procurement decision-making.
| Parameter | Electro-Hydraulic | Electric | Manual |
|---|---|---|---|
| Typical Load Capacity | 250–500 kg | 200–450 kg | 150–250 kg |
| Height Adjustment Range | 620–1,000 mm | 620–1,000 mm | 700–950 mm |
| Trendelenburg Range | ±30° to ±40° | ±30° to ±40° | ±15° to ±25° |
| Lateral Tilt | ±20° to ±25° | ±20° to ±25° | ±15° to ±20° |
| Positioning Speed | Fast, smooth | Fast, precise | Slow, manual effort |
| Battery Backup | 8–12 hours typical | 4–8 hours typical | Not required |
| Radiolucency (C-arm) | Partial (carbon fiber top optional) | Full (standard carbon fiber) | Limited |
| Maintenance Complexity | Moderate (hydraulic fluid) | Low (no hydraulics) | Very low |
| Relative Purchase Cost | High | High–Very High | Low–Moderate |
| Best Surgical Disciplines | General, bariatric, vascular, urology | Orthopedic, neuro, MIS, spine | General surgery, minor procedures |
Beyond the basic table type, a precise specification review is essential. Underspecified tables limit surgical capability; overspecified tables waste capital budget. These are the parameters that should be confirmed for every procurement decision.
Load ratings must be assessed not only as a total weight figure but also as a distributed load specification. A table rated for 300 kg total may only be rated for 180 kg on the head section and 150 kg on the leg section independently. This matters in procedures such as lithotomy positioning, where leg section loads are concentrated. For bariatric surgical programs, a minimum of 450 kg total capacity with distributed section ratings should be the baseline specification, with the tabletop width extended to at least 560 mm (standard tables are typically 500–520 mm wide).
The height adjustment range determines whether a table accommodates both seated surgeons (working low) and standing surgeons of varying heights. A working range of 620 mm to 1,000 mm from floor to tabletop covers the vast majority of surgical team requirements. Floor clearance — the gap between the table base and the floor — should be sufficient for C-arm image intensifier passage; a minimum of 300 mm clearance on at least three sides is necessary for intraoperative fluoroscopy workflows.
Tabletop material selection has direct implications for imaging compatibility, infection control, and patient comfort:
All electrically powered operation tables used in environments where flammable anesthetic agents may be present must meet IEC 60601-1 Class I or Class II electrical safety standards, with CF (Cardiac Float) type protection classification for any components that may contact the patient directly or indirectly. Leakage current to earth must not exceed 100 µA under normal conditions and 500 µA under single-fault conditions. Verify that the table carries CE marking (EU), FDA 510(k) clearance (USA), or equivalent national regulatory approval before procurement.
An operation table's value is significantly defined by the range of surgical positions it can achieve and the accessory ecosystem it supports. No single table can accommodate every surgical discipline without additional positioning aids, but the base table must provide the correct range of motion and attachment points.
| Surgical Position | Table Movement Required | Key Accessory Needed | Common Procedures |
|---|---|---|---|
| Supine | Flat tabletop, height adjustment | Arm boards, safety strap | Abdominal, cardiac, vascular |
| Trendelenburg | Head-down tilt ≥30° | Shoulder braces, anti-slide pad | Pelvic laparoscopy, prostatectomy |
| Reverse Trendelenburg | Head-up tilt ≥30° | Footboard, safety strap | Upper GI laparoscopy, thyroidectomy |
| Lithotomy | Leg section removal or flexion, low height | Stirrups / leg holders (Allen, Yellofins) | Gynecology, urology, colorectal |
| Lateral Decubitus | Lateral tilt, flex break at waist | Lateral positioning pads, kidney rest, bean bag | Thoracic, renal, hip replacement |
| Prone | Flat table, low height for transfer | Wilson frame, chest rolls, Relton-Hall frame | Spine surgery, posterior craniotomy |
| Beach Chair (Semi-Sitting) | Back section elevation 45–80°, leg lowering | Beach chair headrest system | Shoulder arthroscopy, ENT |
Most modern operation tables feature longitudinal side rails — either MAQUET (Trumpf) standard, Skytron standard, or proprietary rails — that accept clamps, arm boards, stirrups, retractor systems, and anesthesia screens. Before selecting a table, confirm that its rail standard is compatible with the positioning accessories already in use in the facility. Mixing rail standards requires adapters that add cost, bulk, and potential instability. A rail-to-rail load capacity of at least 50 kg per clamp attachment point should be verified for heavy retractor systems.
High-volume specialist surgical programs often benefit from dedicated tables optimized for a specific discipline rather than general-purpose tables with add-on accessories. Understanding which specialties justify a dedicated table versus a universal table with accessories is an important strategic decision.
Orthopedic fracture tables are purpose-built for hip and femoral surgery, providing a central post and traction leg attachment that allows traction forces of up to 100 kg to be applied while the patient is fixed. The tabletop is typically split-leg or fully removable to allow C-arm passage for intraoperative fluoroscopy without obstruction. Carbon fiber is standard. A high-volume trauma program performing more than 150 hip fracture operations per year will typically see sufficient efficiency gains to justify a dedicated orthopedic table investment.
Neurosurgical tables feature an integrated, highly adjustable head fixation system — commonly using Mayfield skull clamp attachment — that holds the patient's head rigidly in three-pin fixation during craniotomy. The table must provide extremely fine positioning increments (1° or less for tilt and rotation) and full C-arm compatibility. Electrical safety requirements are particularly stringent due to proximity of neurostimulation equipment.
Urological tables combine a stainless steel or synthetic drainage surface with integrated leg positioning that allows full lithotomy positioning without separate stirrup hardware. Perineal access is maximized by the design. Cystoscopy tables often feature a built-in drainage basin and may include integrated ESWL (Extracorporeal Shock Wave Lithotripsy) compatibility.
Ophthalmic surgical tables are compact, low-height designs that integrate directly with the operating microscope stand. Height range is typically 550–800 mm — lower than general tables — and the head section provides micro-adjustment of head position in all three planes. Anti-vibration design is critical as even minor table vibration can compromise microsurgical precision.
Operation tables are high-touch, high-exposure surfaces in the surgical environment. Inadequate cleaning is a recognized vector for surgical site infection (SSI) and healthcare-associated infection (HAI). A structured cleaning protocol and the correct material selection are non-negotiable.
Not all disinfectants are compatible with all table materials. Chlorine-based agents (bleach) at high concentrations can degrade upholstery and corrode aluminum components over time. Always confirm disinfectant compatibility with the table manufacturer's materials data before establishing a cleaning protocol. Most modern electro-hydraulic and electric tables are rated compatible with quaternary ammonium compounds, accelerated hydrogen peroxide, and isopropyl alcohol up to 70% on all external surfaces.
A properly maintained operation table has a service life of 15–20 years or more. Premature failure is almost always attributable to deferred maintenance, hydraulic fluid neglect, or physical damage to upholstery and sealing surfaces. The following maintenance schedule applies to motorized tables; manual tables require less frequent servicing.
| Interval | Maintenance Task | Applies To |
|---|---|---|
| Daily | Check all functions operate, inspect upholstery for damage, clean and disinfect all surfaces | All table types |
| Weekly | Test battery backup capacity; inspect hydraulic lines for leaks; clean control pendant and cables | Electro-hydraulic, electric |
| 6 Monthly | Full electrical safety test (IEC 60601-1); lubricate mechanical joints; check all locking mechanisms and braking system; inspect castors | All table types |
| Annually | Full preventive maintenance by qualified biomedical engineer; hydraulic fluid change and pressure test; actuator function test; battery replacement if capacity below 80% | Electro-hydraulic, electric |
| Every 2,000 hrs or 2 years | Complete hydraulic system service including seal replacement, filter change, and full system pressure calibration | Electro-hydraulic only |
Applying a structured selection process prevents both undersourcing (a table that limits surgical capability) and oversourcing (paying for capability that will never be used). Work through the following questions in sequence: