Welcome to Jiangsu Yigao Medical
Welcome to Jiangsu Yigao Medical
 E-MAIL:[email protected]
E-MAIL:[email protected]

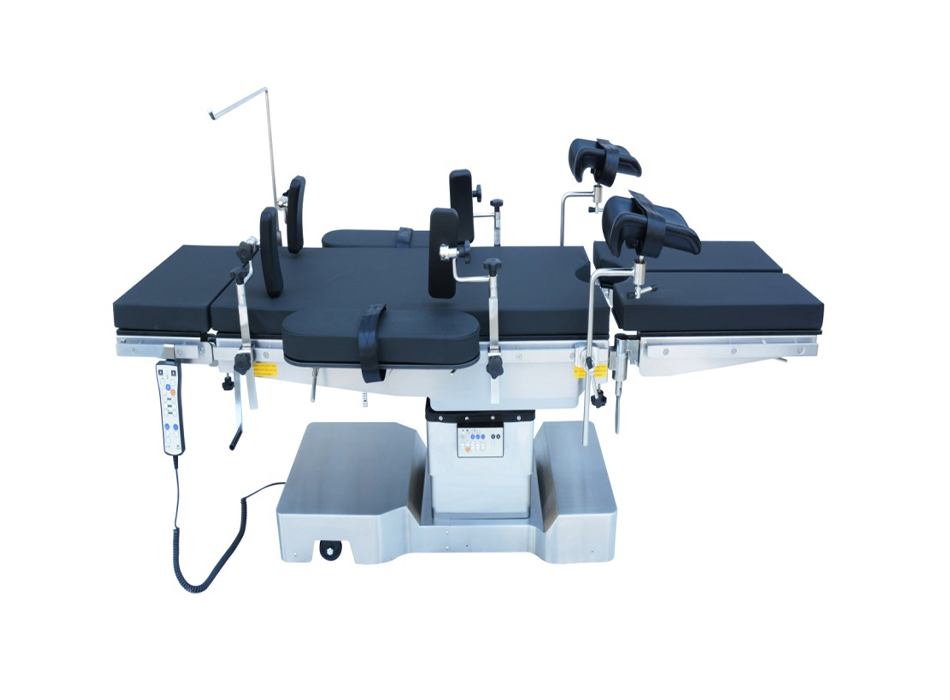
An operating table — also called a surgical table — is a specialized medical platform designed to support a patient in precise, adjustable positions during surgical procedures, providing surgeons with optimal access to the operative site while maintaining patient safety, hemodynamic stability, and pressure injury prevention. The right operating table directly affects surgical outcomes, OR efficiency, staff ergonomics, and patient safety — making it one of the most consequential capital equipment purchases a hospital or surgical center makes.
The global operating table market was valued at approximately $900 million in 2023 and is growing steadily, driven by increasing surgical volumes, aging populations, and the expansion of minimally invasive and robotic-assisted procedures that demand highly precise patient positioning. This guide covers every aspect of operating table selection — types, key technical specifications, positioning systems, imaging compatibility, weight limits, and procurement considerations — so clinical engineers, OR directors, and procurement teams can make fully informed decisions.
No single operating table design is optimal for every surgical specialty. Facilities performing diverse surgical volumes typically maintain multiple table types; specialized centers invest in purpose-built configurations for their dominant procedure mix.
General surgery tables are the most versatile configuration — modular, with interchangeable section inserts and a wide range of positioning capability including Trendelenburg, reverse Trendelenburg, lateral tilt, head-up and head-down, and leg section flex. They accommodate the broadest range of procedures from general abdominal and gynecological surgery to trauma and orthopedic cases. Table height adjustment ranges typically span from 650mm to 1,050mm from floor to table top, accommodating both seated and standing surgical teams and bariatric patients requiring lower transfer heights.
Orthopedic tables are purpose-built for hip arthroplasty, femoral nailing, knee arthroplasty, and spine procedures. They feature radiolucent sections (typically carbon fiber) throughout the working zone to enable fluoroscopic imaging during surgery, with traction devices and limb-positioning attachments that provide controlled mechanical traction to fracture sites. The perineal post assembly and boot traction systems are hallmarks of orthopedic table design. Full radiolucency from head to toe is a non-negotiable specification for orthopedic trauma tables.
Neurosurgical tables prioritize precise, stable head positioning with minimal movement during procedure — any table flex or vibration translates directly to brain movement at the surgical site. They are used with dedicated skull clamp systems (Mayfield, ProneView) that attach to the table head section. Steep Trendelenburg for posterior fossa procedures, lateral positioning for temporal approaches, and prone positioning with chest rolls for spinal procedures all require a rigid, high-precision platform. Many neurosurgical centers use a carbon fiber tabletop across the full length to enable intraoperative MRI or CT imaging without patient transfer.
Ophthalmic tables require exceptional stability and fine positional adjustability — a surgeon working under a microscope cannot tolerate any table drift or vibration. These tables often include integrated microscope arm supports and anti-vibration damping systems. The height range extends lower than general tables — to approximately 450–500mm floor to top — to allow seated microsurgical work. ENT tables add lateral tilt capability for ear and mastoid procedures and chair-like configurations for awake procedures.
Cardiovascular surgery tables must support extended procedures of 4–12 hours or more, integrate with perfusion equipment positioning, and provide exceptional pressure redistribution to prevent pressure injuries during prolonged immobility. Hybrid OR tables — used in facilities combining surgical and interventional radiology capabilities — must be fully compatible with ceiling-mounted X-ray systems (C-arm, flat panel), requiring complete radiolucency and a table column design that does not obstruct the imaging field of view from any angle.
Gynecological and urological procedures frequently require lithotomy position — the patient supine with hips and knees flexed, legs supported in stirrups. These tables feature dedicated articulating leg supports (candy cane, Allen, Yellofin stirrups) that position the legs independently, and steep Trendelenburg capability of 30–40° that is essential for laparoscopic pelvic surgery, improving visualization by displacing bowel superiorly.
Standard operating tables are rated for patient weights of 200–250 kg (440–550 lbs). Bariatric tables extend this capacity to 450–600 kg (990–1,320 lbs) or more, with wider tabletops (typically 580–650mm versus standard 500–530mm), reinforced column structures, wider base footprints for lateral tilt stability, and low transfer heights for safe patient positioning. The bariatric population is the fastest-growing patient cohort in many Western health systems, and inadequate table capacity creates both safety risks and significant legal liability.
Operating table specifications must be evaluated against the actual surgical requirements of the procedures performed in your facility — not against generic "standard" values. The following parameters are the most clinically and operationally significant.
| Specification | Typical Range | Clinical Significance |
|---|---|---|
| Maximum patient load (static) | 200–600 kg | Safety limit; must not be exceeded in any position including tilt |
| Height adjustment range | 560–1,100 mm (floor to top) | Low position for patient transfer; high for surgeon comfort, ergonomics |
| Trendelenburg range | 30–45° head-down | Laparoscopic pelvic surgery requires ≥30°; Fowler position up to 80° |
| Lateral tilt (tilt) | 15–30° each side | Bowel displacement; lateral access; kidney positioning |
| Back section articulation | -30° to +70° (backrest) | Beach chair position for shoulder; chair position for awake procedures |
| Leg section articulation | 0° to -90° (leg lowering) | Lithotomy, Fowler, lateral decubitus positioning |
| Table length (extendable) | 1,900–2,100 mm standard; extendable to 2,300+ mm | Tall patients require head and leg extensions; pediatric inserts for small patients |
| Table width | 500–530 mm standard; 580–650 mm bariatric | Narrow tables improve surgeon access; wider tables required for bariatric safety |
| C-arm / fluoroscopy compatibility | Partial or full radiolucency | Carbon fiber top required for orthopedic, trauma, vascular procedures |
The drive system — how the table is powered to adjust height and position — has significant implications for OR workflow, maintenance requirements, energy consumption, and positioning precision.
Electrically driven tables use electric motors and lead screw or hydraulic actuator systems to adjust all table functions. They offer the most precise, reproducible positioning — critical for neurosurgery, robotic surgery, and stereotactic procedures. Electric tables can store and recall patient position presets, allowing rapid repositioning during multi-stage procedures without manual measurement or guesswork. Electric tables are the standard for most modern ORs due to their combination of precision, speed, and programmability. Battery backup systems maintain full functionality during power interruptions — an important safety consideration for long procedures.
Hydraulic tables use a foot pump or electric pump to pressurize hydraulic fluid that drives the height and tilt functions. They are inherently robust — hydraulic systems are less susceptible to electrical failure and provide high load capacity for their size. The limitation is that hydraulic systems require periodic fluid maintenance (checking fluid level and replacing degraded fluid), carry a small risk of hydraulic fluid leakage, and may drift slightly in position over extended procedures as fluid temperature and viscosity change. They remain common in high-utilization environments where mechanical robustness is valued over positioning precision.
Manual operating tables use hand cranks, levers, and locking mechanisms for all adjustments. They require no electrical or hydraulic systems, making them appropriate for resource-limited settings, field hospitals, and facilities with unreliable power supply. Their disadvantages — slower adjustment, limited positioning range, physical effort for the OR team, and inability to store position presets — make them unsuitable for high-complexity or high-volume surgical centers in well-resourced environments.
Modern electric tables offer multiple control interfaces — each with specific workflow advantages:
Intraoperative imaging — fluoroscopy, C-arm X-ray, CT, and MRI — is used in an increasing proportion of surgical procedures, and the operating table must not obstruct the imaging system's field of view. Imaging compatibility is one of the most technically complex specifications in operating table procurement.
Carbon fiber composite tabletops provide structural strength equivalent to steel while being largely transparent to X-rays — typically providing less than 1mm aluminum equivalent attenuation across the imaging field. Carbon fiber tops are mandatory for orthopedic trauma, vascular, and spine procedures where intraoperative fluoroscopy guides implant placement. They are also required for hybrid OR tables used with ceiling-mounted flat-panel detector systems. The limitation: carbon fiber tops are significantly more expensive than standard foam/upholstery tops and require careful handling to avoid delamination from impact.
The column (pedestal) structure supporting the tabletop determines how freely a C-arm can orbit around the patient. Single-column (monopedal) tables provide the best C-arm access — the column is positioned at the foot or head end, leaving the full length of the patient zone accessible from any angle. Two-column (bipedal) tables have columns at both the head and foot ends, limiting C-arm travel across the full table length.
For hybrid OR and interventional procedures requiring ceiling-mounted imaging systems (rotational angiography, cone-beam CT), the table must provide minimum 400mm clearance beneath the tabletop to allow the imaging gantry to rotate freely around the patient — a specification that eliminates most conventional operating table designs and requires purpose-built angiography or hybrid table platforms.
Intraoperative MRI (iMRI) for neurosurgery and spine procedures requires tables built entirely from MRI-compatible (MR-conditional) materials — no ferromagnetic components whatsoever. These tables must specify MR-conditional status at the specific Tesla rating of the facility's MRI system (1.5T or 3T), as materials acceptable at 1.5T may be unsafe at 3T. iMRI tables are among the most expensive and specialized operating table configurations, costing $150,000–$300,000 or more for complete systems.
Surgical positioning is one of the leading causes of preventable perioperative injury — including peripheral nerve injury, pressure injuries, compartment syndrome, and hemodynamic instability. The operating table must provide the required positioning range while incorporating safety features that protect against positioning-related harm.
Surgical site pressure injuries (SPI) — formerly called intraoperative pressure ulcers — are a recognized patient safety event that prolongs hospitalization, increases costs, and causes significant patient harm. The operating table mattress system is the primary prevention tool.
Surgical procedures lasting more than 2–3 hours carry significantly elevated pressure injury risk — particularly at the sacrum, heels, and occiput. Risk increases further with patient immobility under anesthesia, hemodynamic instability, and low body temperature (which reduces tissue perfusion). Modern operating table mattress systems address this through:
The value of an operating table platform is substantially determined by the range and quality of its accessory ecosystem. Rail systems must accommodate the full range of required attachments with positive locking and no play — accessory movement during surgery is a safety event.
The operating table is a high-contact, high-contamination-risk surface in the surgical environment. Its design must facilitate thorough decontamination between cases and resist degradation from repeated exposure to chemical disinfectants.
Operating tables are classified as active Class II or Class IIb medical devices in most jurisdictions, subject to regulatory clearance before market entry. Key standards and certifications to verify during procurement include:
Operating table purchase decisions involve significant capital investment — standard electric tables cost $20,000–$60,000; specialized orthopedic, neurosurgical, and hybrid OR tables range from $80,000 to $300,000+ — and must account for total cost of ownership over a typical 10–15 year service life.