Welcome to Jiangsu Yigao Medical
Welcome to Jiangsu Yigao Medical
 E-MAIL:[email protected]
E-MAIL:[email protected]

Electric delivery tables are the superior choice for most modern clinical settings, offering hands-free height adjustment, better ergonomic support for both patient and clinician, and enhanced safety features. However, manual delivery tables remain a practical, cost-effective option for facilities with limited budgets or unreliable power infrastructure. The right choice depends on your clinical volume, budget, and care environment.
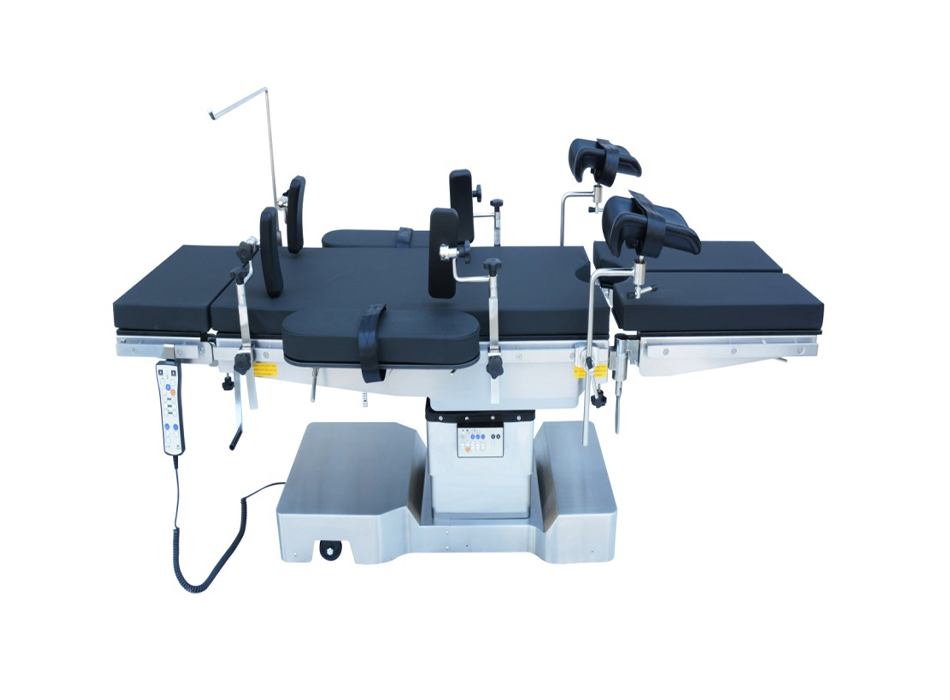
A delivery table — also called a delivery bed or examination bed — is a specialized piece of obstetric equipment designed to support women during labor, delivery, and postpartum examination. Unlike standard hospital beds, delivery tables are engineered with adjustable sections, stirrups, and repositioning capabilities to facilitate vaginal delivery, assisted births, and clinical examinations.
The type of delivery table in use directly impacts clinical outcomes. A poorly designed or malfunctioning table can increase the time staff spend on manual adjustments, raise the risk of patient falls, and contribute to provider musculoskeletal injury. According to occupational health studies, healthcare workers who regularly reposition patients on non-motorized beds face a 35–40% higher risk of lower back injuries compared to those using powered alternatives. Choosing between electric and manual delivery tables is therefore not merely a procurement decision — it is a patient safety and staff welfare consideration.
At the most fundamental level, the distinction between electric delivery tables and manual delivery tables comes down to how adjustments are made — and how fast and precise those adjustments can be during critical moments.
| Feature | Electric Delivery Tables | Manual Delivery Tables |
|---|---|---|
| Adjustment Mechanism | Motorized, foot pedal or remote | Hand cranks or hydraulic levers |
| Height Range | Typically 480–900 mm | Typically 600–850 mm |
| Adjustment Speed | Seconds | 1–3 minutes |
| Power Dependency | Requires AC power or battery backup | None |
| Average Unit Cost | $3,000–$12,000+ | $800–$3,500 |
| Maintenance Complexity | Moderate to high | Low |
| Weight Capacity | 180–250 kg | 120–180 kg |
| Trendelenburg Position | Motorized, one-touch | Manual lever, slower |
In high-acuity delivery scenarios — such as shoulder dystocia, fetal distress, or emergency C-section preparation — every second counts. This is where the performance gap between electric and manual delivery tables becomes most apparent.
Electric delivery tables allow clinicians to reposition a patient into the Trendelenburg, lithotomy, or flat supine positions in under 10 seconds using a foot pedal or wireless handset. This hands-free operation means providers can maintain sterile technique while repositioning — a critical advantage during assisted deliveries or when managing postpartum hemorrhage.
Many modern electric delivery tables also feature memory presets, allowing staff to store preferred positions for specific providers or procedures. Facilities that have switched from manual to electric delivery beds report a reduction in repositioning time of up to 70%, with measurable improvements in team coordination during obstetric emergencies.
Manual delivery tables do not depend on electricity, making them indispensable in rural clinics, field hospitals, or regions with inconsistent power supply. Their mechanical simplicity means fewer failure points — a hand crank or hydraulic pump will not suddenly malfunction mid-procedure the way a motor or control board can.
However, the physical effort required to adjust a manual delivery table during an active delivery can disrupt clinical focus. Staff must divert attention from the patient to operate levers or cranks, and in bariatric cases, heavy loads can make adjustments physically demanding or slow.
The ergonomic impact of delivery table selection is frequently underestimated in procurement decisions, yet it has significant implications for staff retention and long-term operational costs.
When calculating total cost of ownership, facilities should factor in potential reductions in worker compensation claims and sick leave associated with upgrading from manual to electric delivery beds. In some cases, the long-term savings in staff injury costs offset the higher upfront investment within 3–5 years.
From the patient's perspective, the delivery bed is where some of the most vulnerable and physically demanding moments of childbirth occur. Comfort, stability, and smooth repositioning all affect the birth experience.
Electric delivery tables move smoothly and at a controlled pace, reducing jarring or sudden shifts that can be distressing during active labor or immediately postpartum. Manual tables, by contrast, may move in increments depending on the lever or crank mechanism, which some patients find uncomfortable.
Electric tables typically include integrated side rail controls, anti-Trendelenburg locks, and low-height settings (as low as 480 mm) that reduce the distance from bed to floor — a key factor in fall prevention guidelines. Patient falls from delivery tables represent a significant liability risk, and lower minimum height settings directly reduce fall-related injury severity.
With rising rates of maternal obesity globally — the WHO estimates that over 30% of women of reproductive age are overweight or obese in high-income countries — bariatric capacity is increasingly relevant. Electric delivery tables commonly support up to 250 kg, while many manual examination beds are rated only to 150–180 kg, limiting their applicability in this growing patient population.
Purchase price alone does not tell the full financial story. A comprehensive cost comparison must account for maintenance, longevity, staff injury costs, and operational efficiency.
| Cost Category | Electric Delivery Table | Manual Delivery Table |
|---|---|---|
| Initial Purchase | $5,000–$12,000 | $800–$3,500 |
| Annual Maintenance | $200–$500 | $50–$150 |
| 10-Year Maintenance Total | $2,000–$5,000 | $500–$1,500 |
| Estimated Staff Injury Savings | $1,500–$4,000 (per table) | $0 |
| Typical Service Lifespan | 10–15 years | 8–12 years |
For high-volume maternity units performing 500+ deliveries per year, the efficiency gains of electric delivery tables — faster room turnover, fewer staff reassignments, smoother workflows — translate into measurable time savings that compound over years of operation. For smaller clinics with fewer than 100 deliveries annually, a well-maintained manual delivery table may represent sufficient capability at a fraction of the cost.
Electric delivery tables are the recommended option when one or more of the following conditions apply:
Manual delivery tables and examination beds remain highly appropriate in specific contexts:
Whether selecting an electric or manual delivery table, certain specifications should be assessed for every unit under consideration:
The comparison between traditional and electric delivery tables ultimately resolves around three variables: clinical complexity, facility volume, and resource availability. Electric delivery tables outperform manual alternatives on nearly every clinical and ergonomic metric, but their advantages only justify the cost in settings where those capabilities will be regularly utilized.
For hospitals and high-volume maternity centers, investing in electric delivery beds is a sound long-term decision that pays dividends in staff safety, patient experience, and operational efficiency. For smaller clinics, outpatient examination settings, or environments where power reliability is uncertain, a well-specified manual delivery table or examination bed remains a clinically appropriate and financially prudent choice.
In all cases, procurement decisions should be made with input from clinical staff who use the equipment daily — their practical experience will surface priorities that no specification sheet can capture.